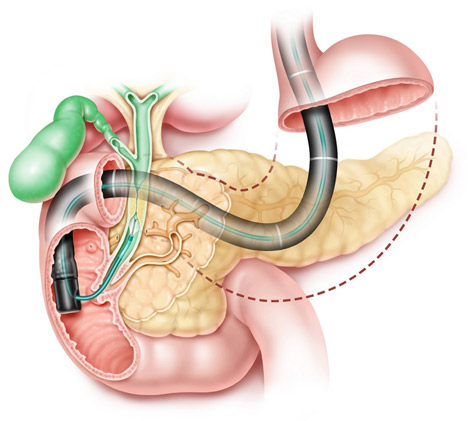
ERCP
ERCP (short for endoscopic retrograde cholangiopancreatography) is a procedure used to diagnose diseases of the gallbladder, biliary system, pancreas, and liver. The test looks “upstream” where digestive fluid comes from – the liver, gallbladder, and pancreas – to where it enters the intestines. In addition, ERCP can be used to treat problems in these parts of the digestive system.
During an ERCP, a gastroenterologist (doctor who specializes in treating diseases of the gastrointestinal system), uses a special endoscope (a long, flexible tube with a light and camera at the end) to examine the inside of the digestive system. The doctor identifies the place where the bile duct comes into the intestine and then feeds a tiny catheter (a plastic tube) into the duct and squirts in a contrast agent while X-rays are taken. The contrast agent allows the doctors to see the bile ducts, the gallbladder, and the pancreatic duct on the X-rays.
Once the source of the problem is identified, the doctor may then treat it by performing one of the following procedures.
- Sphincterotomy. This involves making a small incision (cut) in the opening of the pancreatic duct or the bile duct, which can help small gallstones, bile, and pancreatic juice to drain appropriately.
- Stent placement. A stent is a drainage tube that is placed in the bile duct or the pancreatic duct to hold the duct open and allow it to drain.
- Gallstone(s) removal. ERCP can remove gallstones from the bile duct, but not from the gallbladder itself.
An ERCP is considered a low-risk procedure; however, complications can occur. These can include pancreatitis, infections, bowel perforation, and bleeding. Patients undergoing an ERCP for treatment, such as for gallstone removal, face a higher risk of complications than patients undergoing the test to diagnose a problem. Your doctor will discuss the risks of possible complications before the test.